Health insurance benefits—
a Headway Guide

How benefits work
When you sign up for an insurance plan, you agree to a contract. Typically, you pay a monthly premium, or fee, to your insurer, and in exchange, that insurer covers various costs related to your care. This can include anything from a routine office visit to a trip to the emergency room. Having an insurance plan can give you peace of mind by keeping your monthly costs predictable and manageable, even in the event of an unexpected health cost.
For each plan, some providers are considered in-network, while others are out-of-network. This status impacts how much you’ll pay for care.
In-network
A provider is in-network if they accept your insurance plan. You can check to see if a mental health provider is in-network with your plan directly from Headway’s website.
Headway’s goal is to greatly expand the number of in-network providers across all insurance plans nationwide.
or
Out-of-network
A provider is out-of-network if they do not accept your insurance plan.
Note that some insurance plans may still pay for part of the cost of an out-of-network provider, but you will save less money by choosing them.
If you’re booking on Headway, you’ll only be able to book with in-network providers.
Today, most plans include some sort of coverage for mental health care. That said, some do not. You can check your mental health coverage for your current plan by doing any of the following:
- Enter your insurance plan details on Headway to see if we can instantly verify
- Visit your insurance company's website or app
- Review your EOB (explanation of benefits) and look for details on "behavioral health benefits"
- Call your insurance company directly to ask
How much you pay and why
If your plan includes mental health benefits, these factors will typically have the greatest impact on what you pay. Headway works with your insurance company to understand these parts of your plan and determine your cost per session.
Deductible
A deductible is a set amount of money you must spend before your insurer pays for some of your care. With these plans, the out-of-pocket price per session is set by your insurance company. Once you’ve reached your deductible amount, your insurance company will start to contribute to your therapy costs. The percentage they then pay is determined by your plan.
Copay
A copay is a flat rate per session set by your insurance plan. With a copay, you’ll pay the same amount for each session regardless of type or length. Your insurer covers the rest.
Coinsurance
The coinsurance is the percentage of the session cost you're responsible for paying after your deductible’s been met. Your insurance covers the remaining percentage. For example, if your coinsurance is 10%, you pay 10% and your insurer pays 90% of the session cost.
Out-of-pocket max
Your out-of-pocket max is the most money you’ll pay for in-network care in a given plan cycle (a cycle usually lasts 1 year). In most cases, once you reach this number, you’ll no longer need to pay a copay or coinsurance, and you’ll owe $0 per session, until your plan resets for a new cycle.
Why costs change
Over the course of a year, your in-network costs per visit will often go down as you progress through your plan. This is because most plans cover more of your costs the more you spend. That said, your costs can sometimes go up as well. Here are two examples:
1. Your cost per session decreases for future sessions. This usually happens when you reach your deductible or out-of-pocket max, which means your insurance plan is working as intended! You’ll benefit from lower costs for the rest of your plan cycle.
2. Your cost per session suddenly goes back up. Typically, this happens because your plan cycle just ended and your benefits reset. For many plans, this happens on January 1, but it can vary depending on your particular insurer or employer. This means your plan is working as intended, and you’ll usually only pay this higher cost temporarily
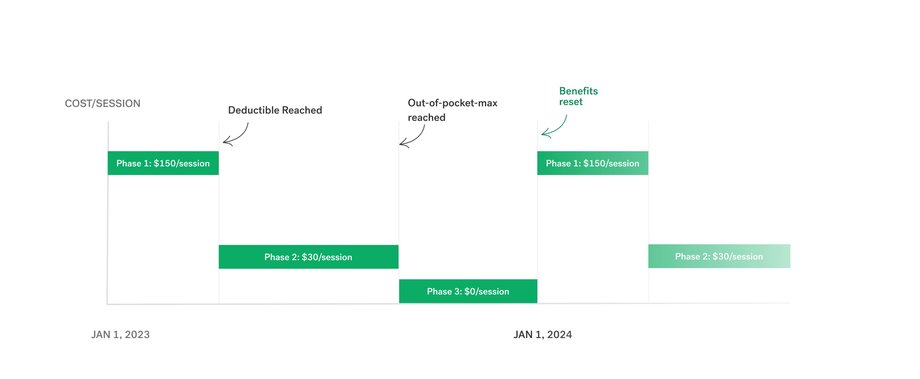
As a combined example of the two cases above, consider a fictitious client named Jane. Note that all of these dollar amounts will vary depending on the plan.
- Phase 1: Jane starts the year paying full cost ($150) for each therapy session.
- Phase 2: After paying $150 for 10 sessions, she reaches her deductible of $1,500. She must now only pay a 20% coinsurance per session, or $30. Her insurer covers the remaining 80% ($120).
- Phase 3: Later in the year, Jane has spent enough of her own money on therapy to reach her out-of-pocket max. Her insurer covers the full cost of each session for the rest of the year, and Jane pays $0 per session.
- Back to Phase 1: Jane's plan resets on January 1, and she goes back to paying $150 per session until she reaches her deductible again in her new plan cycle.

When your insurance benefits reset, usually around January 1st, cost changes and plan updates can get confusing. Our team is here to help make these changes as easy to understand as possible, and to get you an accurate cost as soon as we can.

Sithara
Insurance operations at Headway
Benefit resets
As outlined above, your session cost might temporarily increase when your benefits reset. You can confirm with your insurer or ask your employer to double check your reset date to confirm this is what happened. That said, a few other situations tend to occur during benefit resets that are a bit more complicated. Here are some common things that can happen after a reset, and what you can do in each case.
Benefit resets and what you can do
Helpful resources
Other commonly asked questions
Getting help
Headway is here to provide the support you need.
Find answers to common questions from Headway clients
If you're already a client on Headway, you can review your latest benefits here.
For additional questions about compliance or Headway in general, contact our support team.
Disclaimer
This document should be used for general informational purposes only. The contents do not constitute legal or health advice and should not be used as a substitute for advice from legal counsel or a medical professional. Use this page as a reference guide, not as a definitive source of information regarding health insurance plans.